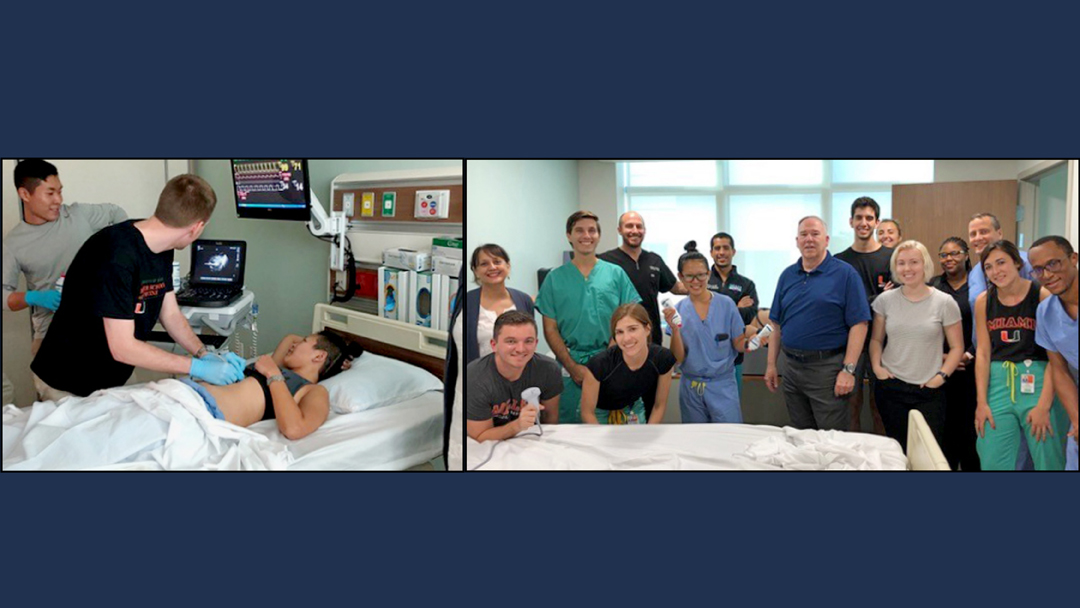
Ultrasound Student Interest Group: A Model for Active Learning & Multi-Specialty Collaboration
Our success as an interest group is due not only to great mentorship, but also to the engagement of faculty and students from specialties beyond emergency medicine. We have reached our largest membership base, serving 177 students across all four classes—nearly 25% of our medical student body.
A Brief History of Ultrasound Education
In recent years, the use of point-of-care ultrasound (POCUS) has exploded. Medical ultrasonography was developed as an imaging modality a half-century ago, originally to non-invasively search for tumors and other growths in the World War II era. [1] Since then, not only have the capabilities of POCUS evolved with the advancements of image optimization techniques, transducers and Doppler, but its applications have also expanded dramatically across many medical specialties.
Unfortunately, current clinical utilization of POCUS in healthcare settings is limited, mostly due to the operator’s unfamiliarity with the instrument and the lack of formal education. Although POCUS training has been incorporated as a residency requirement by some specialties— such as emergency medicine, obstetrics and gynecology, and internal medicine, to name a few—its integration and standardization as a part of a medical school curriculum is highly variable.
In a 2012 survey of MD-granting accredited medical schools in the U.S., 62.2% reported that ultrasound education was integrated into their curriculum in at least one of the four years, either as a tool to teach basic science and medicine concepts or to teach students how to obtain ultrasound scans. [2] Historically, at the University of Miami Miller School of Medicine (UMMSM), ultrasound education is offered as a third-year elective, and only recently within the past academic year has ultrasound been introduced to first-year students.
As second-year medical students at UMMSM, our interest in POCUS in all its glory stems from its easy and rapid usability, portability, little-to- no-risk of radiation, and low cost to the patients we serve.
USIG at UMMSM: The Beginnings
Concurrent with the development of POCUS as a robust diagnostic and procedural tool in clinical practice, Ultrasound Student Interest Groups (USIGs) have emerged as popular extracurricular entities. These not only augment the medical school curriculum, but also help students develop the skills necessary to become comfortable with ultrasonography. Furthermore, medical school administrations have also begun to pay heed to the student demand for integrating ultrasound into the formal curriculum. Of note this year, the University of California, Irvine became the first medical school to purchase handheld ultrasound machines for every student. [3]
Given the shortfall of ultrasound education in our medical school curriculum, our USIG was created three years ago at the Miller School of Medicine as a student organization with officer positions held by second-, third- and fourth-year medical students, and under the guidance of the Emergency Ultrasound Director at Jackson Memorial Hospital’s Emergency Department in Miami. Our mission has been to promote and expose students to the use of ultrasound, including acquiring and interpreting ultrasound scans, and to demonstrate its integration across many specialties with the intent of creating student leaders in ultrasound. Participation in USIG activities has been voluntary and open to first- through fourth-year students.
What is particularly unique about our USIG this year is that we have incorporated the gamification model of active learning into our organ system-focused workshops, and also we have expanded our collaboration with a wide array of other student interest groups.
The primary means by which our USIG engages and informs student members is through workshops that focus on the application of ultrasound to particular organ systems. In order to promote student involvement and active learning, our workshops are designed on the principles of “gamification.”
Similar to published literature, we define gamification as “the process of game-thinking and game mechanics to engage users and solve problems.” [4,5] Gamification is a new genre of teaching that has risen in popularity in the 21st century, and it is being utilized by a variety of professional specialities. [6,7] Cell phone applications, group competitions and video games are being adapted from social hobbies outside of the classroom to serious learning mechanisms in the realm of higher education. [6,7,8,9] Indeed, this mechanism of learning has been shown to be advantageous in promoting motivated learning and improved task performance. [6]
A core component to learning ultrasound must be a direct “hands-on” experience due to the complex ultrasonographic stereoscopy involved with imaging internal anatomy. Learning through gamification has been supported by research in teaching similar stereoscopic procedural hospital interventions, such as chest tube placement and laparoscopic surgery. [10,11]
We find gamification to lend itself to learning POCUS by promoting persistence, creativity, risk taking and self-direction. We have created several games for our workshops. The “Mirror Image Challenge” in our Respiratory Workshop and the “Fast FAST Exam” in our Gastrointestinal Workshop have been very successful.
In the “Mirror Image Challenge,” teams of students were instructed to reproduce a referenced ultrasound image using an ultrasound machine on a live model. Teams then saved and submitted their best-acquired image. All students voted on the best-acquired ultrasound image that matched the original (of course, students could not vote for their own image). This task challenged students to learn how transducer and machine manipulations of angle, depth and gain could be optimized in the acquisition of images. Furthermore, the spirit of competition and the announcement of the winning team incentivized student effort and achievement through extrinsic motivation.
In the “Fast FAST Exam,” pre-selected teams of students learned how to perform the FAST exam for 30-minutes on human models. Teams then played each other for the fastest time to obtain the standard views of the FAST exam.
Anonymous, self-reported student feedback from our workshops has shown overwhelmingly positive support for learning ultrasound through games. More specifically, 87.5% (n=8) of students reported a rating of >4 out of 5 as their level of enjoyment of the “Fast FAST exam” and 100% (n=10) of students reported a rating of >4 out of 5 for the “Mirror Image Challenge.”
Collaborations
Our success as an interest group is due not only to great mentorship, but also to the engagement of faculty and students from specialties beyond emergency medicine. We have reached our largest membership base, serving 177 students across all four classes—nearly 25% of our medical student body. We believe our growth can be best attributed to our expanded reach, offering students exposure to a range of ultrasound applications.
The following interdisciplinary workshops are offered:
-Echocardiogram Workshop in the Echo Lab – Cardiology Interest Group
-GI Workshop with FAST Exam – Trauma Surgery Interest Group
-Ultrasound-Guided Amniocentesis – The Vagina Monologues & Ob-Gyn Interest Groups
-“How to Nerve Block” – Student Interest Group in Anesthesiology
-Ultrasound of Soft Tissue – IDEA Clinic, a wound care clinic associated with a needle exchange
-Ultrasound in Clinical Simulation – Medical Simulation Interest Group
-Ultrasound Table at the EM Symposium – Emergency Medicine Student Association
Our USIG has strongly advocated for incorporating ultrasonography into the official medical school curriculum. One of our major accomplishments has been partnering with the head teaching assistants of the anatomy course to organize ultrasound labs that utilize ultrasonography to augment the first-year medical students’ anatomy curriculum.
At the heart of these collaborations has been our persistence to make non-traditional connections, to contribute to ultrasound implementation into medical curriculum, and to foster a love for ultrasound in as many students as possible, exemplifying that ultrasound is for everyone. ■
References
- Goldberg BB, et al. Early History of Diagnostic Ultrasound: The Role of American Radiologists. American Journal of Roentgenology 1993;160:189-194. Available at: www.ajronline.org/doi/pdf/10.2214/ajr.160.1.8416623
- Bahner DP, et al. The State of Ultrasound Education in U.S. Medical Schools: Results of a National Survey. Academic Medicine 2014;89(12): 1681-1686. Available at: medicine.hofstra.edu/pdf/faculty/facdev/ultrasoundinusmedicalschools.pdf
- Comstock J. UC Irvine Medical School gifts Butterfly handheld ultrasounds to its whole class of 2023. MobiHealthNews 2019. Available at: www.mobihealthnews.com/news/north-america/uc-irvine-medical-school-gifts-butterfly-handheld-ultrasounds-its-whole-class
- Zichermann G, Cunningham C. Introduction. Gamification by Design: Implementing Game Mechanics in Web and Mobile Apps. Sebastopol, CA: O’Reilly Media, Inc; 2011:xiv
- McCoy, Lise; Lewis, Joy H.; Dalton, David W. Gamification and Multimedia for Medical Education: A Landscape Review. The Journal of the American Osteopathic Association. Jan. 2016; Vol. 116 (No. 1).
- Michael Sailer, et al. How gamification motivates: An experimental study of the effects of specific game design elements on psychological need satisfaction. Computers in Human Behavior, Vol. 69 (2017)
- Lombardi MM; Oblinger DG, ed. Authentic Learning for the 21st Century: An Overview. Louisville, CO: EDUCAUSE Learning Initiative; 2007.
- Gorbanev, louri, et al. A systematic review of serious games in medical education: quality of evidence and pedagogical strategy. Medical Education Online. 2018.
- Edwards EA, et al. Gamification for health promotion: systematic review of behaviour change techniques in smartphone apps. BMJ Open. 2016 Oct 4.
- Haubruck, P., et al. Evaluation of App-Based Serious Gaming as a Training Method in Teaching Chest Tube Insertion to Medical Students: Randomized Controlled Trial. Journal of Medical Internet Research. 2018; 20(5), e195. doi:10.2196/jmir.9956
- Ju, R., et a. Comparison of Nintendo Wii and PlayStation2 for enhancing laparoscopic skills. JSLS: Journal of the Society of Laparoendoscopic Surgeons. 2012. 16(4), 612–618. doi:10.4293/108680812X13462882737294
This article is part of the following sections: